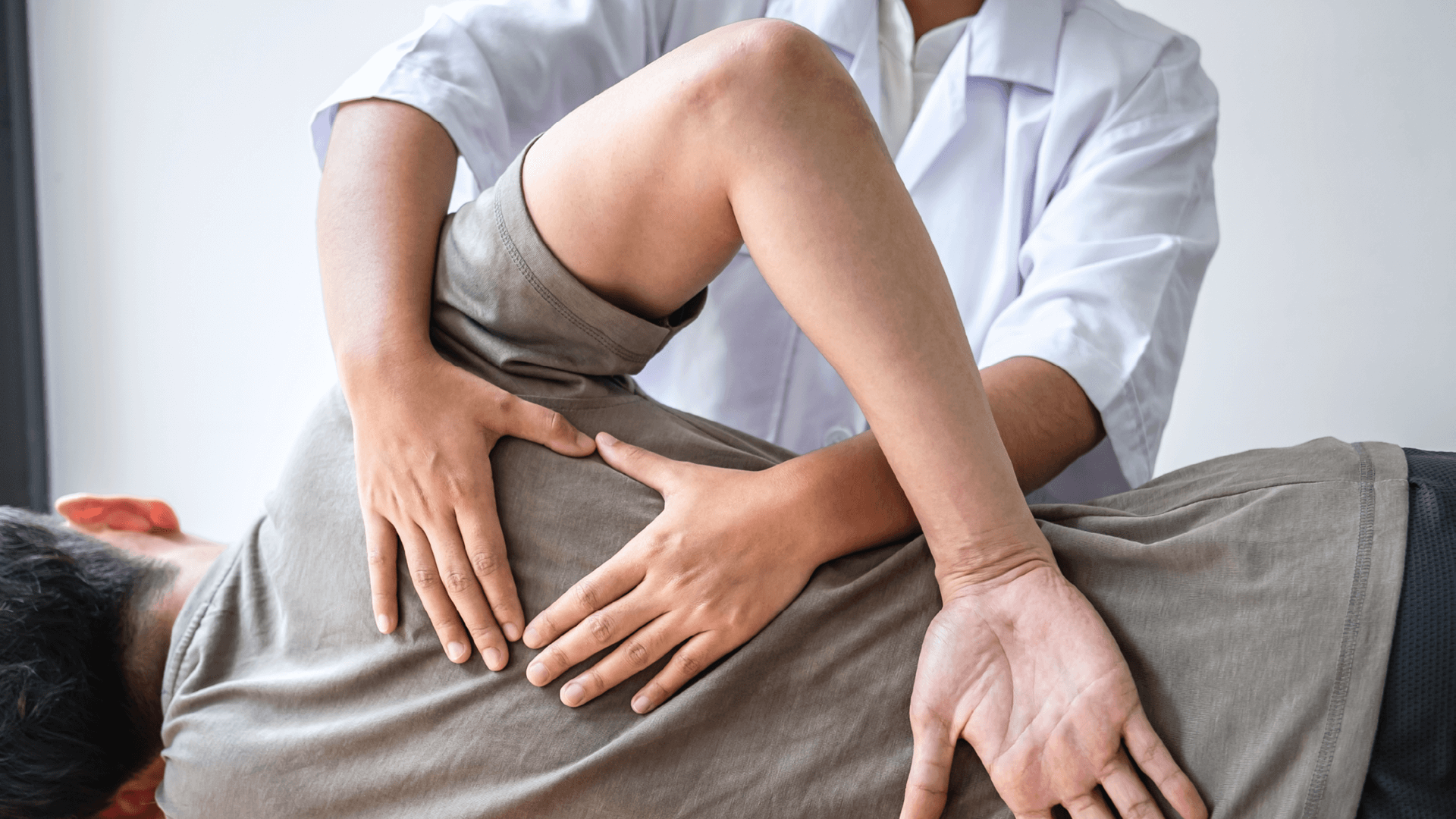
Whether you are seeking massage or giving massage – do you know what you are looking for or understand what you are giving. When seeking massage therapy, people often hear the terms Remedial Massage and Sports Massage and wonder about the differences. Though both modalities aim to restore and enhance physical function, they have different intents – and this is probably the most important word (intent). Let’s delve into what sets sports and remedial massage means and who benefits from each (or both).
My personal journey in bodywork was shaped by a background in sports and recreation management, over 20 years of training in Japanese martial arts, and time served as a sports trainer in local clubs. Everything that I do is about living – movement is living, and movement is meant to be fun! As a remedial massage therapist, I want to support you to do the things you love with the ones you love the most.
In my practice, I work with recreational road runners at varying levels, from beginners to marathon and ultra- runners. I also work with cyclists and triathletes (sports that I participate in) to assist them to reach their personal goals. And curiously, I have a small following of pole dancers (which is not a sport of mine).
Public Perceptions vs. Reality
There’s a common belief that Remedial Massage is the “massage that hurts” and “the one that I can claim a rebate from my health fund on”. On the other hand, Sports Massage is the massage that men get (because it sounds more masculine) – and needs to be hard and fast. But these stereotypes only scratch the surface of what these therapies involve.
What is Remedial Massage?
Medibank has provided this definition for Remedial Massage. The systematic assessment and treatment of muscles, tendons, ligaments, and connective tissues to assist in rehabilitation, pain relief, and injury management. It involves:
- Assessment-Driven Treatment: Identifying the root cause of pain or dysfunction.
- Flexible Techniques: A therapist may employ a range of techniques and tools which might include hands on soft tissue techniques, and it may also include use of tools such as dry needling, cupping, or myofascial release.
- Restorative Intent: The aim is to support the body’s own healing processes and restore normal function.
You will notice that in the accepted definition there is no mention of any specific modality, technique, pressure or pain.
While the title isn’t protected or registered, a Remedial Massage Therapist would usually hold a Diploma of Remedial Massage from an Australian Registered Training Organisation.
The focus of a Remedial Massage Therapist isn’t always on sport. A remedial massage therapist might be a generalist, working with “anyone”. However, many choose a specific focus based on their experiences, ongoing training and world view. This could include working in areas like palliative care, oncology, or occupational rehabilitation. Others might focus on specific conditions like TMJD, Parkinson’s disease, or recovery from frozen shoulder.
A person seeking remedial massage might engage in treatment for a few sessions, or for a chronic or life-altering injury/illness require ongoing care.
Attending your remedial massage you can expect the therapist to ask you:
- Complete an intake form
- Ask you about your health history – including your current symptoms and history of those symptoms
- Why you are attending massage and what else you have tried (and the outcome)
- And many other questions
- Discuss treatment options with you
- Undertake an assessment
- Perform a remedial massage treatment and assess the outcomes
- Inform you of a recommended course of treatment or refer you on to another professional
Sports Massage: Tailored for Athletic Performance
Sports Massage is not just a post-match rub down or any specific technique or modality. It’s an approach designed to enhance and maintain an athlete’s physical capabilities. A sports massage can still be remedial in nature. The intention is that a sports massage aims to:
- Support training and training programs
- Prepare for Competition: Get the athlete ready to perform
- Support Recovery: Help muscles recover post-training or post-competition.
- Prevent and Treat Injuries: Address sport-specific injuries or strains.
This might include very conservative work to support participation or competition, through to very detailed and intentional work including specific assessment and management. Therapists might work with athletes in general or they may have a specific knowledge set and personal experience working with a particular sport – e.g. swimmers, hockey players, baseballers, runners. These athletes will usually develop consistent and predictable patterns (which if unmanaged may lead to injury) based on the repeatable nature of their activities.
Many sports massage therapists may or may not hold a diploma of remedial massage, with many massage training schools holding sports massage training in their Certificate level programs. They may have gone on to work alongside other allied health professionals in high performance settings, and many have also undertaken additional training through Sports Medicine Australia.
The work of a sports massage therapist could range from a rub down at the side of a track during training sets for a cyclist, to specific muscle and soft tissue care for example management of a cuff injury to support the injury recovery of a swimmer. An experienced sports massage therapist would be aware of the training program of the athlete and should also be observing training and be in communication with the coach and other allied and allied adjacent therapists.
Attending your sports massage, you can expect the therapist to ask you about:
- Your sport and level of participation
- Where you are at with your training program
- When is your next match / competition or training goal
- Your coach and other supporting health professionals
- Why you are seeking massage treatment
- Who have you already seen and what was the result
- How best to work with you and when to work with you to meet your goals
- And many other questions – including performing an assessment before and after treatment – especially in the instance of restriction or injury
In a true high-performance setting, an athlete often has a team of professionals—coaches, trainers, strength and conditioning coaches, physiotherapists, nutritionists and sports psychologists—dedicated to every aspect of their well-being. These athletes have the resources and time to focus intensely on recovery and rehabilitation.
However, it’s different for a recreational or self-funded athlete. These individuals juggle training with work, family, and other demands. Their resources, including time and money, are divided, which influences how they can commit to their recovery.
For a therapist, this means acknowledging these limitations and managing expectations. It’s about finding ways to integrate recovery strategies into an athlete’s busy life, recognising that they might not have the same support network as an elite AFL footballer or AIS scholarship funded swimmer.
Qualifications and Therapist Focus
In Australia, the most common qualifications for massage therapists include:
- Certificate IV in Massage Therapy: Provides foundational training, sometimes with a focus on sports massage techniques.
- Diploma of Remedial Massage: Offers more comprehensive training in anatomy, physiology, and injury management. Therapists with this qualification are better equipped to assess and treat complex issues.
- Some States also offer even higher levels of education through Advanced Diplomas and Undergraduate Degrees in Soft Tissue Therapy and Myotherapy.
Choosing the Right Approach for You
When deciding between Remedial and Sports Massage, consider your goals and needs. If you’re experiencing pain or restricted movement, or if you require a tailored approach to restore function, a Remedial Massage may be the best fit. On the other hand, if you’re an athlete preparing for a competition or recovering from an intensive training session, Sports Massage might be more appropriate.
Watch out for charlatans – the title of massage therapist is not protected, and anyone can call themselves a massage therapist whether they have no training, just a little bit of training or a lot of training. When choosing your massage therapist ask them about their:
- qualifications
- association membership
- insurance
- commitment to ongoing training
- experience in your sport / activity / injury